For Lisa-May Shaw, growing up in Newman in the Pilbara meant community, resilience and wide-open skies. She lived there until she was 17 before moving to Bunbury then Perth in 2009, where she built what she describes as a “normal city life working in corporate environments”. It was in Perth that she met her husband Casey and, in 2019, they made the decision to return to his family farm, swapping corporate offices for paddocks and long horizons.
By 2021, Lisa-May was fully immersed in rural life, working in admin for a local grower group. Like many regional families, they have faced their share of challenges, including losing their home during Cyclone Seroja. Rebuilding became part of their story, strengthening their connection to community and to the land they had chosen to return to.
Then came their son Henry in 2022, followed by daughter Penelope in 2024. These days she manages the bookwork for the farm while raising their two young children, her world centred firmly on family.
“Since moving to the farm and becoming a mother I feel like I’ve stepped into a whole new rat race,” she says. “One that has no direction and involves 25 snacks a day and endless washing.”
She laughs, but there’s honesty in it. “I’ve never really been career driven, so having kids has felt like it’s become my purpose.”
In late 2024, that purpose was tested in a way no parent ever expects. At just two years old, Henry became critically unwell, and within hours their world shifted.
In the weeks leading up to his diagnosis, there had been small signs. Nappies soaked through more often than usual, constant thirst, always hungry.
“I Googled the symptoms,” Lisa-May admits. “Type 1 diabetes appeared on the screen, but it felt unlikely. He was only two.”
When Henry became lethargic and struggled to breathe one Tuesday morning, instinct took over. At the local hospital, a finger prick test revealed blood glucose levels of 26 and high ketones of 6 (normal levels are between 4-10 for blood glucose and under 0.6 for ketones). He was in diabetic ketoacidosis (DKA), a medical emergency.
“At that point we still didn’t really know much other than Henry was very sick,” she recalls.
Within hours, the Royal Flying Doctor Service was on its way. Henry was classified as a Priority 1 retrieval and flew to Perth that night with Casey by his side.
“Casey could not have spoken more highly of the staff on the plane,” Lisa-May says. “They explained everything that was happening and what would happen next. It helped him process it all.”
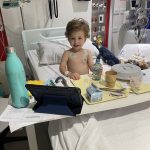 Henry spent his first night in ICU at Perth Children’s Hospital before moving to the ward. What followed was a week in hospital, multiple education sessions and the beginning of a steep learning curve. At the time of diagnosis, Penelope was just six months old.
Henry spent his first night in ICU at Perth Children’s Hospital before moving to the ward. What followed was a week in hospital, multiple education sessions and the beginning of a steep learning curve. At the time of diagnosis, Penelope was just six months old.
“Our sleepless nights became even more sleepless,” Lisa-May says. “We were up every three hours checking Henry’s glucose levels.” A continuous glucose monitor helped after the first week, but the early days were still overwhelming. “It was information overload while you’re still trying to process the diagnosis.”
Living regionally adds layers to an already complex condition. Every three months, the family travels to Perth for clinic appointments, a rhythm that will continue until Henry turns 18. When he has been unwell with viruses, insulin requirements spike as his body fights infection. Gastro brought further hospital stays, with regional teams liaising closely with Perth specialists.
“We’re incredibly grateful for our local hospital and doctors,” Lisa-May says. “But there are limits to what’s available regionally.”
Even routine care requires planning. Dental treatment must often be done at Perth Children’s Hospital so his glucose levels can be closely monitored if fasting or anaesthetic is required. School has required specialised training for teachers to manage his pump and glucose monitoring. Every snack must be carefully calculated, recipes tested before being packed into lunchboxes. An untested or miscalculated snack can result in large spikes or drops that can take a long time to resolve.
“You can’t just hand him food,” she explains. “You’re always counting carbohydrates, always thinking about what it’s going to do to him.”
Sleep is often interrupted by high and low blood glucose alarms that demand immediate attention. High glucose levels affect his mood and energy. The mental load rarely switches off. “The biggest emotional adjustment is knowing it’s forever,” she says. “You hope there might be a cure one day, but you also have to accept that this is his life.”
There are moments that tug hard at a mother’s heart, explaining to a toddler why he cannot eat freely when he feels desperately hungry during a low glucose event, or navigating the reality that sleepovers are not simple because extended family need training and confidence to manage his care. “I do feel mum guilt that he’s had to adapt to this. It’s not a small thing, it’s lifelong.”
And yet, Henry continues to show them what resilience truly looks like.
“He’s taught us how resilient and brave he is,” Lisa-May says. “Kids are so adaptable. As long as we show him things are okay, that we’re not worried or afraid, he’s not worried. He just accepts it and goes with the flow. We are so proud of him.”
What she wishes more people understood is simple. Type 1 diabetes is not caused by too much sugar. It is not preventable. It is not the same as Type 2.
“His pancreas just doesn’t work,” she says plainly. “There’s still that old-school thinking that diabetes is caused by a bad diet. I remember someone asking if he had Type 1 or Type 2, and it just shows that there’s such a lack of understanding around the differences between Type 1 and Type 2. Prior to this we didn’t really understand either so it would be great to see more awareness and understanding.
Henry is not defined by diabetes. He is a little boy who plays, learns, laughs and lives, just with a little something extra to manage.
For rural mums facing a sudden diagnosis or medical emergency, Lisa-May’s message is clear and deeply personal.
“Don’t blame yourself,” she says. “I was so angry at myself for not taking him in earlier, but we were told most toddlers end up in DKA before they’re diagnosed and we weren’t alone in those feelings. Trust your gut. If something feels wrong, get it checked. The worst that can happen is being told they’re healthy. Lean on your family. Know your child will be okay. You will get through it, even if it feels like you won’t.”
In regional WA, distance can feel vast. But so is strength.
For Lisa-May and her family, that strength now lives in the quiet, daily act of showing up, counting carbs, setting alarms, driving long roads to appointments, and choosing every single day not to let a diagnosis define their son’s future.

